At a Glance:
| What it TMJ Botox: A therapeutic Botox treatment that relaxes overactive jaw muscles (such as the masseter and temporalis) responsible for clenching, grinding, and muscle-driven TMJ pain. How it helps: By reducing excessive muscle activity, TMJ Botox eases pressure on the jaw joint, lowers headache frequency, and protects teeth from grinding-related wear. What to expect: Quick in-office injections, minimal discomfort, no downtime, and gradual relief that typically begins within days and peaks in about two weeks. |
Do you wake up with jaw pain, morning headaches, or facial soreness?
You’re not alone. These could be signs of TMJ disorder.
Jaw pain, clenching, and teeth grinding aren’t just uncomfortable; they can slowly damage your teeth, strain your facial muscles, and trigger chronic headaches.
TMJ Botox® is a targeted, non-surgical treatment that relaxes overactive jaw muscles to reduce pain, tension, and bruxism, with no downtime.At Yaletown Dental Boutique, TMJ Botox is used as a therapeutic dental treatment, not a cosmetic shortcut. It’s carefully planned, conservatively dosed, and often combined with other TMJ solutions, such as nightguards or bite adjustments, for long-term relief.

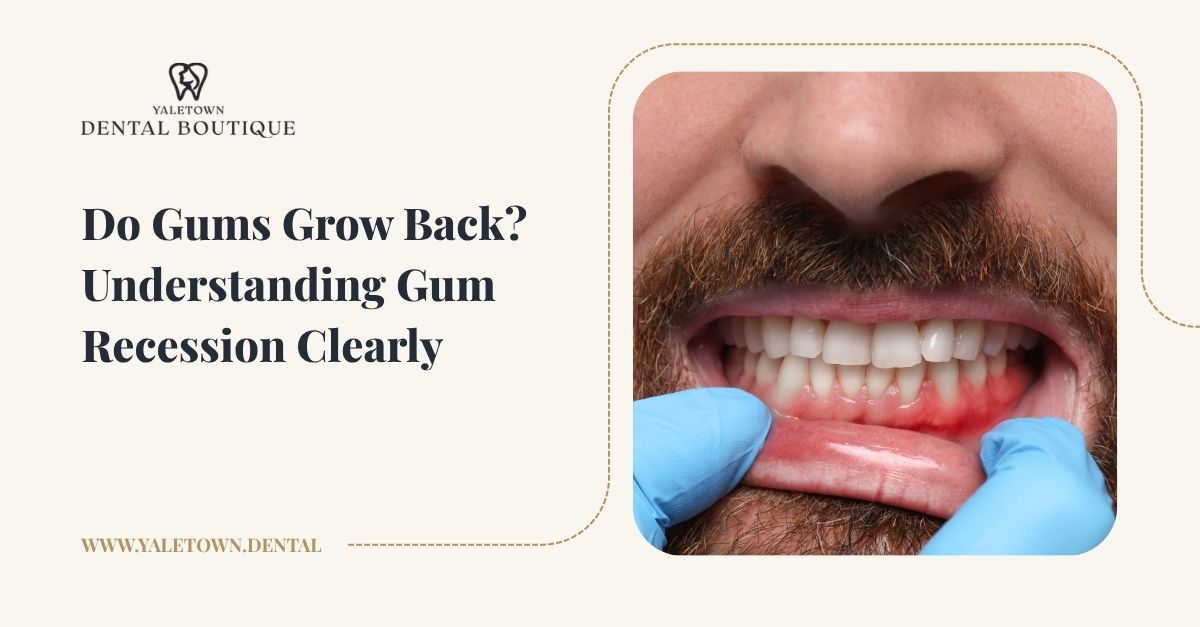
What is TMJ disorder?
The temporomandibular joint (TMJ) is the hinge that connects your jawbone to your skull, located just in front of each ear. It allows you to chew, speak, yawn, and make facial expressions.
When the joint or surrounding muscles become inflamed, strained, or misaligned, it can lead to TMJ disorder, also known as TMD. This condition can cause pain, tightness, and difficulty moving the jaw.
Instead of a long explanation, here’s the key context most patients need:
TMJ Disorder: Quick Context
What’s Happening
TMJ symptoms often come from muscle overuse, joint stress, or bite imbalance rather than a single injury.
Common Triggers
Jaw clenching, teeth grinding (bruxism), stress, poor posture, arthritis, or past trauma to the jaw or neck.
Why It Lingers
Overactive muscles can keep the joint under constant pressure, making symptoms persist even when the joint itself looks “normal” on imaging.
Why Treatment Varies
Some patients need bite support or physiotherapy, while others benefit most from muscle-relaxing therapies like Botox, especially when clenching and grinding are dominant factors.
TMJ Botox works best when muscle overuse is the main driver of pain. It’s not a cure-all; it’s part of a smart, personalized treatment plan.
What causes TMJ disorder?
There’s no single cause of TMJ disorder. In most cases, it results from a combination of muscle tension, joint issues, or lifestyle habits that disrupt how the jaw functions.
The TMJ relies on smooth cartilage and a small shock-absorbing disc to move comfortably. When any part of this system becomes irritated, worn down, or out of alignment, it can lead to pain, stiffness, and reduced jaw mobility.
Here are some of the most common causes of TMJ disorder:
- Jaw Clenching and Teeth Grinding (Bruxism): Constant clenching, often during sleep or under stress, overloads the jaw muscles, keeping them in a tight state and increasing joint pressure.
- Chronic Muscle Overuse: Habits like chewing gum, nail biting, or holding tension in the jaw can fatigue the masseter and temporalis muscles, leading to pain and spasms.
- Stress and Anxiety: Emotional stress commonly shows up in the jaw. Many patients clench unconsciously throughout the day, reinforcing the pain–tension cycle.
- Bite Imbalance or Jaw Misalignment: When the bite doesn’t distribute forces evenly, certain muscles work harder to compensate, often triggering TMJ symptoms over time.
- Disc Displacement or Erosion: The small disc inside the joint can slip out of place or wear down over time. This often causes clicking, popping, or even jaw locking.
- Joint Damage from Arthritis: Conditions like osteoarthritis or rheumatoid arthritis can wear away joint cartilage, leading to inflammation, stiffness, and long-term discomfort.
- Injury or Trauma to the Jaw or Neck: A blow to the face—such as from a fall, accident, or sports injury—can strain or misalign the TMJ and surrounding structures.
- Sprains or Strains in Soft Tissues: Overuse of the jaw muscles and ligaments through clenching, over-chewing, or poor posture can create chronic strain and pain.
Because muscle overactivity plays such a central role, treatments that directly relax these muscles can significantly reduce pain, clenching, and tension when other approaches haven’t been enough.
At Yaletown Dental Boutique, we take the time to understand the unique causes behind your symptoms. Using digital scans and advanced diagnostics, we create a personalized care plan that may include Botox therapy, bite correction, or other treatments designed to support long-term relief.
What is TMJ Botox & how does it work?
Botox, short for botulinum toxin, is a purified protein derived from a bacterium called Clostridium botulinum. While it can be harmful in high doses or unregulated settings, medical-grade Botox is carefully refined, diluted, and sterilized to make it safe for therapeutic use.
TMJ Botox is a therapeutic dental treatment that targets the overactive jaw muscles responsible for clenching, grinding, and tension-related pain. Rather than treating symptoms on the surface, it works at the source of muscle overload that drives many TMJ cases.
How TMJ Botox Works
Botox temporarily blocks the nerve signals that tell specific muscles to contract forcefully. When those signals are reduced, the muscle can finally relax.
Result: Less clenching → less pressure on the jaw joint → reduced pain, tension, and headaches.
For many TMJ patients, the biggest driver of pain isn’t the joint itself; it’s muscle overactivity. Botox allows those muscles to rest and reset.
Targeted Muscles in TMJ Botox
TMJ Botox is not injected randomly. It’s placed precisely into muscles proven to contribute to TMJ symptoms:
- Masseter Muscle (jaw angle): Primary clenching and grinding muscle; often enlarged and overworked.
- Temporalis Muscle (temples): Common source of tension headaches and jaw fatigue.
- Supplementary Muscles (When Needed): In some cases, supporting muscles of the jaw or neck may be treated to improve balance and comfort.
Why This Matters for TMJ Relief
By calming these muscles:
- Jaw tension decreases,
- Teeth grinding is reduced,
- Pressure on the TMJ joint eases.
- And headaches and facial soreness often improve.
TMJ Botox does not freeze your face or affect expression when performed correctly. It’s a functional, targeted treatment designed to restore comfort, not change how you look.
Is TMJ Botox effective?
While Botox isn’t a cure for TMJ disorder, growing evidence supports its use as a treatment, especially when other methods haven’t helped.
Botox is typically considered when options like splints, medications, or physiotherapy provide little relief. It works best for patients whose symptoms are caused by jaw clenching, muscle overuse, or teeth grinding.
TMJ Botox works best when symptoms are primarily muscle-based, including:
- Chronic jaw tightness or fatigue
- Nighttime clenching or grinding (bruxism)
- Tension headaches linked to jaw muscles
- Facial soreness without major joint damage
What the Research Says
Several studies have found that Botox can significantly reduce jaw pain, improve movement, and ease related symptoms:
One study involving 44 participants showed that pain decreased by 59% after one month, and by 70% after six months of treatment.1
Another smaller study reported that patients experienced fewer headaches and improved jaw mobility for up to three months following Botox injections.2
Additional research, including a 2003 study, found that up to 90% of participants who didn’t respond to other treatments saw improvements after trying Botox.3 While these results are promising, researchers still call for larger, long-term studies to fully understand how effective Botox is for TMJ in the general population.
Part of a Multi-Modal TMJ Plan
At Yaletown Dental Boutique, we stay informed on the latest TMJ treatment options. If you’re struggling with pain or limited jaw function, Botox could be a safe, targeted way to regain comfort and improve quality of life.
It’s most effective when combined with other TMJ-focused strategies, such as:
- Bite analysis and occlusal adjustment
- Night guards or splints (when indicated)
- Physiotherapy or posture support
- Stress and habit awareness (clenching triggers)
This multi-modal approach helps ensure Botox provides relief and supports long-term jaw stability.
Many TMJ symptoms are driven by chronic jaw clenching or nighttime grinding rather than structural joint damage.
Patients who want to understand this option in more detail can review our dedicated page on Therapeutic Botox for grinding in Yaletown, which explains how treatment fits into a broader TMJ care plan.

Benefits of TMJ Botox
Botox offers several key advantages for people dealing with TMJ-related pain, tension, and grinding, especially when other treatments haven’t worked.
Here’s what many patients experience:
- Fast Relief: Most people start to feel improvement within a few days to two weeks after treatment. For many, the reduction in jaw pain and tightness is noticeable and lasting.
- Long-Lasting Effects: Results usually last three to four months, with consistent improvements in comfort and jaw mobility over time.
- Less Clenching and Tension: By calming overactive muscles, Botox eases tightness in the jaw, temples, and face, helping break the pain cycle.
- Fewer Tension Headaches: Jaw tension is a major cause of chronic headaches. Botox often reduces their frequency and intensity.
- Protects Teeth: Less grinding means reduced wear, cracking, and stress on teeth, restorations, and the jaw joint itself.
- Minimal Downtime: The procedure is quick, non-surgical, and requires no recovery time. Most patients return to normal activities the same day.
- Safe When Performed by Experts: When administered by trained professionals, like our team at Yaletown Dental Boutique, Botox is a safe, controlled treatment with very low risk of side effects.
These benefits make TMJ Botox a practical option for patients seeking relief without surgery, medications, or long interruptions to their routine.
What happens during the procedure?
Botox treatment for TMJ is a quick, non-surgical procedure performed right here at Yaletown Dental Boutique. Most sessions take 10 to 30 minutes and involve little to no discomfort.
1. Assessment
Your visit begins with a focused discussion about your symptoms: jaw pain, clenching, headaches, or grinding. Your dentist evaluates jaw movement and identifies the muscles contributing most to your discomfort.
2. Muscle Mapping
Key muscles are carefully mapped, most commonly the masseter (jaw) and temporalis (temples), and, in some cases, the surrounding facial muscles. This step ensures Botox is placed only where it’s needed.
3. Micro-Dose Injections
Using a fine needle, small, controlled amounts of Botox are injected into the targeted muscles. Most patients describe the sensation as a brief pinch, and the entire injection process usually takes just a few minutes.
The number of injections depends on your symptoms and muscle activity. In some cases, a treatment plan includes multiple sessions spaced over several months for optimal relief.
4. Aftercare Guidance
You can return to normal activities immediately after your visit. However, we recommend:
- Avoiding rubbing or massaging the injection sites
- Staying upright for at least four hours
- Waiting until the next day before exercising
Most patients feel noticeable relief after a few days, with full results within two weeks.
5. Review at 2–3 Weeks
Relief often begins within days, with full results developing over one to two weeks. A follow-up review around the 2–3 week mark allows your dentist to assess improvement and fine-tune the plan if needed.
At Yaletown Dental Boutique, we make sure the entire experience is as comfortable, safe, and personalized as possible, from consultation to follow-up.
Who is a good candidate?
TMJ Botox is most effective when symptoms are caused by muscle overuse, clenching, or grinding rather than joint damage alone. A routine dental exam allows your dentist to assess jaw movement, muscle activity, and bite patterns to determine whether Botox is an appropriate part of your TMJ treatment plan.
You may be a good candidate if you:
✔ Experience chronic jaw pain, tightness, or facial soreness
✔ Clench or grind your teeth (bruxism), especially during sleep
✔ Have frequent tension headaches linked to jaw strain
✔ Haven’t found lasting relief with night guards, physiotherapy, or medication
✔ Want a non-surgical option with minimal downtime
✔ Are looking to reduce muscle-driven TMJ symptoms safely and predictably
Defer or avoid TMJ Botox if:
⚠ You are pregnant or breastfeeding
⚠ You have certain neuromuscular conditions (e.g., myasthenia gravis)
⚠ There is an active infection or inflammation at the injection site
⚠ You have known allergies to botulinum toxin products
⚠ Your jaw pain is primarily caused by advanced joint degeneration rather than muscle activity
If Botox isn’t appropriate right now, that doesn’t mean you’re out of options. Your dentist can recommend alternative treatments or help address underlying issues first so you can revisit TMJ Botox safely in the future.
Safety & Side Effects
TMJ Botox is considered safe when administered by trained dental professionals using precise, conservative dosing. Most patients tolerate treatment well and return to normal activities the same day.
Common (Usually Mild & Temporary)
These effects are expected shortly after treatment and typically resolve on their own within a few days.
- Tenderness or soreness at injection sites
- Mild bruising or swelling
- Jaw fatigue as muscles begin to relax
Uncommon (Usually Dose- or Placement-Related)
These side effects are less common and are usually temporary when they occur.
- Temporary smile asymmetry
- Chewing fatigue, especially with harder foods
- Localized muscle weakness near the treated areas
Aftercare
Simple aftercare steps help reduce side effects and support optimal results.
- Avoid rubbing or massaging injection sites for 24 hours
- Stay upright for at least 4 hours after treatment
- Avoid strenuous exercise until the next day
- Follow any personalized instructions provided by your dentist
If anything feels unusual or doesn’t improve as expected, your dental team can reassess and guide next steps.
How long does TMJ Botox last?
TMJ Botox works gradually, with relief building over time and lasting for several months. Understanding the timeline helps set realistic expectations and plan follow-up care if needed.
Treatment Timeline
TMJ Botox doesn’t work instantly, but it follows a clear and predictable pattern as the muscles gradually relax and tension reduces over time.
3–7 Days: Onset of Relief
In the first few days after treatment, jaw muscles begin to relax. Early signs often include reduced tightness, less clenching, and milder morning soreness.
~2 Weeks: Peak Effect
By about two weeks, Botox reaches its full effect. Most patients notice the greatest reduction in jaw pain, tension, headaches, and teeth grinding at this stage.
~3–4 Months: Duration of Results
Results typically last three to four months, depending on muscle strength, clenching habits, and individual response. As muscle activity slowly returns, symptoms may gradually reappear.
Many patients choose repeat treatments to maintain consistent relief, especially if TMJ symptoms are chronic or stress-related.

Start Feeling Better—Explore TMJ Botox Today
Jaw pain, clenching, and tension don’t have to be something you live with every day. If TMJ symptoms are affecting your comfort, sleep, or quality of life, a proper assessment is the first step toward relief.
At Yaletown Dental Boutique in Yaletown, TMJ Botox treatment always begins with a comprehensive evaluation of the jaw and muscles. This allows us to confirm whether your symptoms are muscle-driven and determine if Botox is the right option or if another approach would serve you better.
📞 Call us at 604-900-8005
📅 Book your TMJ assessment online
Our team will walk you through your options, explain what to expect, and create a personalized plan focused on long-term comfort, not just temporary relief.
How long does TMJ Botox last?
The effects typically last three to four months, depending on your muscle activity and the severity of your symptoms.
Are there any side effects?
Most side effects are mild and temporary. These can include slight swelling, bruising, or tenderness at the injection site. Rare side effects may include dry mouth or muscle weakness near the treated area.
Can a dentist administer Botox for TMJ?
Yes. In British Columbia, licensed dentists with appropriate training can safely administer Botox for both therapeutic and cosmetic purposes.
Will TMJ Botox affect my smile or facial expressions?
When properly placed in targeted jaw muscles, Botox should not change your smile or natural expressions. Precision dosing is key.
Is TMJ Botox a permanent solution?
No. TMJ Botox is not permanent. It’s a symptom-management treatment often used as part of a broader care plan that may include bite therapy or habit management.